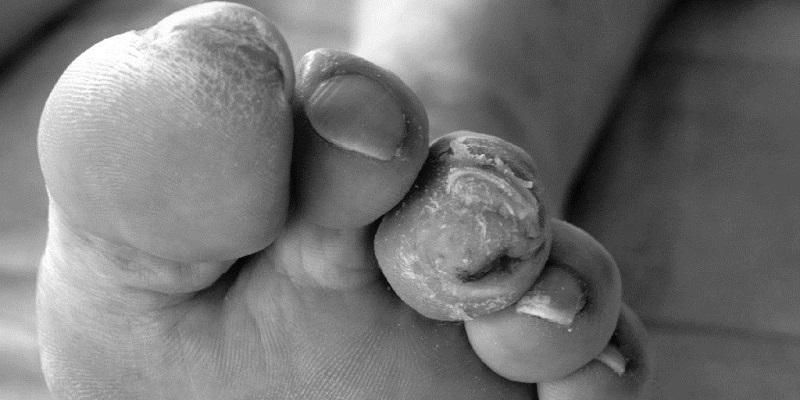
The prognosis for people with an infected diabetic foot ulcer is worse than was previously thought, according to new research.
More than half the patients in the research study did not see their ulcer heal after a year – and one in seven had to have part or all of their foot amputated.
Foot ulcers are open wounds and they affect around a quarter of the 3.3 million people in the UK living with diabetes.
The wounds develop because diabetes damages the nerves and blood vessels in the feet.
These wounds are chronic, slow to heal and prone to infection, and it is infection that normally leads to some of the severe consequences such as losing a limb or multiple amputations.
Need for close monitoring
The research, led by Professor Andrea Nelson at the University of Leeds, set out to examine the outcomes for people with infected diabetic foot ulcers and the results underline the need for people at risk of foot ulcers to be closely monitored.
Not only do the ulcers cause disability, there are big financial implications for the NHS. The National Institute for Health and Care Excellence or NICE puts the annual cost for treating diabetic foot wounds at £650 million.
“The results of our study should help clinicians identify those most at risk of poor outcomes so that we can look to provide further support.”
The University of Leeds is at the forefront of research into preventing and treating diabetic foot ulcers as well as skin wounds and pressure sores more generally, a problem that affects people with poor circulation, obesity or limited mobility – and one that is expected to grow as society gets older.
This latest study is published in the journal Diabetic Medicine.
The researchers tracked 299 people who had attended a diabetic clinic with an infected foot ulcer, a big enough sample for it to be representative of the picture across the UK.
The patients were followed up a year later and by then, one in seven people (17.4 per cent) had part or all of their foot amputated.
Among the others, less than half (45.5 per cent) had seen their ulcer heal. The researchers say the outcomes were worse than previously thought – a conclusion based on a more accurate statistical analysis of the scale of the problem.
Professor Nelson from the Faculty of Medicine and Health said: “Foot ulcers are a very nasty condition. They’re painful and are debilitating. People with foot ulcers have limited mobility, and that brings with it a whole set of other risk factors – obesity and heart disease, for example.
“The key point is that people need to be seen quickly if an ulcer begins to form – that gives health workers the greatest chance of trying to treat the condition.”
Dr Michael Backhouse, a podiatrist and Senior Research Fellow at the University of Leeds, said: “The results of our study should help clinicians caring for patients with diabetes to identify those most at risk of poor outcomes so that we can look to provide further support.”
The research was funded by the National Institute for Health Research.
Wound care research
The University of Leeds has a long tradition of research activity regarding wounds, such as pressure ulcers or bed sores, leg ulcers as well as diabetic ulcers.
Researchers working at the University of Leeds have been involved in many studies informing current practice about pressure ulcer prevention using specialist beds and mattresses - and leg ulcer care, such as the use of compression therapy for treating venous leg ulcers.
Much of this research has been done in partnership with nurses in Leeds.
Research into practice
The University will next week host a one-day conference and public events in partnership with Leeds Teaching Hospitals NHS Trust looking at wound care over the last 100 years.
The conference will look at the latest science and research of wound care and also at the history of wound care via the experience of nurses who served in the First World War.
Professor Nelson will present the latest work on wound infection and Dr Una Adderley, also from the School of Healthcare, will discuss the current evidence around leg ulceration.
Half of all people with a leg ulcer do not receive a diagnosis of the cause of their leg ulcer so may not receive appropriate treatment.
Dr Adderley said: “The NHS is starting to address this gap in practice. But there is a fairly urgent need to get clinicians working in the community to ensure their patients get the right treatment, and that can make a big difference to people with leg problems.”
The University is also involved in the Legs Matter campaign to raise awareness about, and early treatment for, leg ulcers.
The conference and public events on Friday 17 November are free to attend but registration is compulsory via this Eventbrite page.
Further information
For media enquiries email the University of Leeds Press Office at pressoffice@leeds.ac.uk.