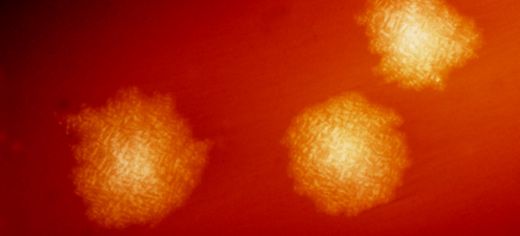
More than 39,000 cases of the hospital bug Clostridium difficile are missed in Europe each year because of a lack of clinical suspicion or inadequate lab testing, a Europe-wide study led by University of Leeds experts has found.
Findings from an international study into Clostridium difficile incidence (CDI) were presented at the 24th European Congress of Clinical Microbiology and Infectious Diseases in Barcelona this week.
Data from 482 European hospitals reveals that in a single day, an average of 109 cases of CDI are missed due to a lack of clinical suspicion or inadequate laboratory testing, potentially leading to more than 39,000 missed cases in Europe each year.
“Countries with increased awareness of CDI have been able to improve early diagnosis and reduce outbreaks associated with the most virulent strains of CDI,” said Professor Mark Wilcox, Professor of Medical Microbiology at the University of Leeds.
“This study highlights that it is essential that we improve the implementation of testing in hospitals, in order to tackle the issue of the increasing incidence of the bug across Europe.”
The European multi-centre, prospective bi-annual prevalence study of Clostridium difficile infection in hospitalised patients with diarrhoea (EUCLID) involved 482 hospitals from 20 European countries.
These full results compare data captured on two separate days, one in winter 2012/13 and one in summer 2013. On each of the assigned days, participating hospitals submitted all samples of unformed faeces to the 20 EUCLID national coordinating laboratories (NCL) across Europe. In total, 7,181 faecal samples were submitted by participating hospitals.
Results of this study highlighted marked recent shifts in CDI testing policy and methodology across Europe, resulting in improved testing policies and selection of laboratory methods. The data shows that false-positive rates decreased between the two study days in those countries where testing procedures and methods had improved.
Despite this, more than 50% of hospitals are still not using the most accurate testing procedure for CDI and more than one in five (21.8%) samples found to be positive for CDI at the NCL had not been tested at local hospital level. In addition, the findings reveal that more than half (52.1%) of hospitals in Europe only test for CDI at a doctor’s request.
“Guidelines exist recommending hospitals test for CDI in all unformed stools of which the cause is undetermined. However we are still seeing an issue with both a lack of clinical suspicion and lack of testing for CDI”, said Professor Wilcox. “CDI is a condition which causes considerable suffering for patients and is a huge economic burden to hospitals across Europe. These results reveal that there is still more to be done in order to optimise CDI management and prevention.”
The study was funded by pharmaceutical company Astellas Pharma Europe Ltd.
Further information
Professor Mark Wilcox is available for interview. Please contact Ben Jones in the Press Office on 0113 34 38059 or email B.P.Jones@leeds.ac.uk