
Expensive high-tech air mattresses are only marginally better at preventing pressure sores and ulcers than a specialist foam mattress, according to the results of a major study.
Known as alternating-pressure mattresses, the high-tech devices contain air pockets which inflate and deflate to constantly change pressure points on the skin. They cost at least £1,000 each.
In comparison, a specialist foam mattress costs about £200 and is made up of high-quality polyurethane and viscoelastic foam designed to cradle the patient to reduce pressure on the skin.
The specialist foam mattresses are in widespread use across the National Health Service, while the high-tech air mattresses are found on approximately 10% of NHS hospital beds and given to patients considered to be at high risk of pressure ulcers – even though there has been no independent evaluation of their effectiveness.
The UK Government’s health regulator, the National Institute of Health and Care Excellence (NICE), had called for a scientific trial to investigate the benefits of the high-tech mattresses.
That study, led by nurse researchers at the University of Leeds, is published today in the journal EClinicalMedicine (published by The Lancet).
Clinical benefit
The investigation showed that the gains from the use of the high-tech air mattresses were marginal. The paper concludes that for every 50 patients allocated to one of the high-tech air mattresses, only one would benefit from it.
The results showed that 6.9% of patients on the high-tech air mattresses developed a pressure sore that was grade two (i.e. blister or break in the skin) or worse compared with 8.9% on the specialist foam mattress. Ulcers are graded on a scale from one to four, with four being the most serious.
The median length of time it took for the ulcers to develop for the patients on a high-tech air mattress was 18 days, compared to 12 days for those on the specialist foam mattress.
The paper also noted that the overall number of patients that developed pressure sores during the study was smaller than expected: the result, the researchers believe, of changes in nursing practice designed to reduce the burden of pressure sores.
This is the first large-scale study world-wide into the effectiveness of high-tech air and specialised foam mattresses to prevent pressure sores. It involved more than 2,000 patients at high risk of developing pressure sores in hospital and NHS community units.
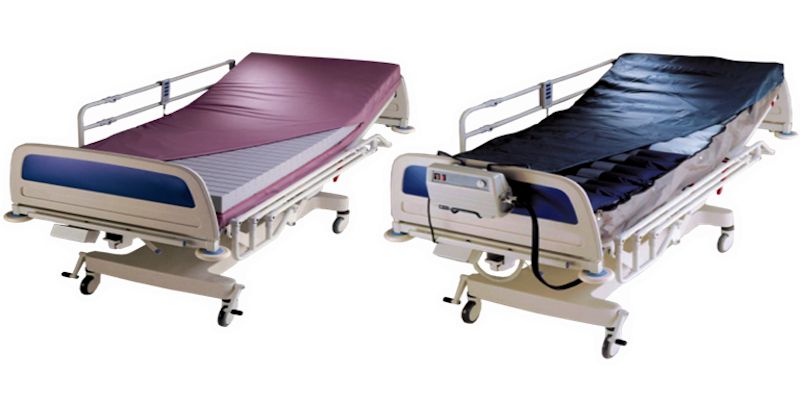 A specialist foam mattress (left) and an alternating-pressure air mattress (right)
A specialist foam mattress (left) and an alternating-pressure air mattress (right)
In 2018, NHS Improvement described pressure sores as a “concerning and avoidable harm” with the costs to the NHS of treating the condition running at more than £3.8 million every day.
Pressure sores are a major complication faced by people who are bedridden or immobile. The pressure that builds on soft tissue causes distortion to the tissues and/or an interruption to the blood supply – and that kills or damages skin leading to painful ulcers.
The study was led by Professor Jane Nixon, from the University of Leeds' Institute of Clinical Trials Research.
She said: “The professional guidelines tell healthcare staff that they should use specialist foam for all at-risk patients and high-tech air mattresses for patients with an existing pressure ulcer when adequate pressure distribution cannot be achieved.
“But in practice, some nurses provide high-risk patients as well as those with existing pressure ulcers with the high-tech air mattresses and there has not been any evaluation of the effectiveness of one type of mattress over another.
“Some patients find the air mattress unsettling. They are kept awake by the noise of the pump, feel unsafe because the mattress is moving, or just find them uncomfortable.
“Rehabilitating patients also complain that they can’t move around themselves or get in and out of bed – and that exacerbates already limited mobility.”
Patients who agreed to take part were randomly allocated to either a high-tech air or specialised foam mattress for two months or until discharge, whichever came sooner. They were then assessed by a nurse for a final time 30 days after discharge. The majority of the patients were elderly, with the median age 81, and included a number of patients who were aged over 100.
The analysis suggested that the patients who benefitted most from the high-tech air mattresses were those who were completely immobile, confused, had nutritional deficits or very red skin on a pressure area.
Financial evaluation
The study found an economic advantage to using the high-tech air pressure mattresses. Although they cost more to buy, the patients who were nursed on them had, on average, a slightly shorter stay in hospital, and that reduced the overall cost of care. More research is needed to fully understand the correlation between mattress type and length of hospital stay.
While acknowledging there were benefits to using the high-tech air pressure mattresses, the researchers said that as the gains were small, advice to nurses should be that most patients could be safely cared for on a specialised foam mattress.
Professor Nixon said: “The outcome of this study provides the evidence that specialist foam mattresses are appropriate for most patients who are at high risk of developing pressure ulcers.
“But staff should be free to exercise clinical discretion in provision of either mattress, informed by patient preference, comfort or rehabilitation needs, as well as specific risk factors such as being completely immobile, being confused, having nutritional deficits or early signs of pressure damage.”
The study was funded by the UK National Institute of Health Research Health Technology Assessment programme and supported by the Pressure Ulcer Research Service User Network.
Further information
For media enquiries email the University of Leeds Press Office at pressoffice@leeds.ac.uk.
The paper, ‘Pressure relieving support surfaces for pressure ulcer prevention: clinical and health economic results of a randomised controlled trials’, is published in the journal EClinicalMedicine, and available online at: https://doi.org/10.1016/j.eclinm.2019.07.018
Other researchers involved in the trial were from Leeds Teaching Hospitals NHS Trust, University of Exeter Medical School, Leeds Community NHS Trust and Mid Yorkshire Hospitals NHS Trust.