A new clinical intervention trial aims to improve outcomes for patients with the bone marrow cancer multiple myeloma (MM).
The UK-wide study, led by researchers at the University and funded by Cancer Research UK, has been welcomed as a “great breakthrough” by leading sector charity Myeloma UK.
Those taking part in the UKMRA Myeloma XIV FiTNEss trial will have been newly diagnosed with MM and focuses on patients deemed unsuitable for intensive therapy.
The new study aims to determine whether modifying treatment based on patients’ frailty can keep them on medication for longer and improve their results.
“This trial has the potential to change how we practice delivering care in our clinics.”
Each year about 5,000 people are diagnosed with the illness, with some two thirds aged 70 and over.
Research shows that patients who receive intensive therapy including stem cell transplantation have the best outcomes, with younger and fitter patients generally living more than six years after diagnosis.
But frailty and fitness levels mean many are deemed transplant non eligible (TNE) – leading to poorer outcomes for people who are less fit or aged over 75.
The trial will involve 740 patients from approximately 90 hospitals across the UK. It is led by the Leeds Institute of Clinical Trials Research – part of the University’s School of Medicine – with funding from Millennium Pharmaceuticals Inc (Takeda).
Takeda and Celgene, a Bristol Myers Squibb pharmaceutical company, are providing drugs free of charge for the duration of the trial.
Gordon Cook, Professor of Haematology and Myeloma Studies and Clinical Director (Haematology) at Leeds Institute of Clinical Trials Research, said: “This is the only trial globally looking to test if a clinical score can identify vulnerable patients at risk of treatment-related toxicity and modifying how we deliver therapy up-front rather than in response to developing side effects, which is the standard of care.
“The international myeloma community is eager to see the outcomes from this trial, which has the potential to change how we practice delivering care in our clinics.”
Previous trials in TNE patients – where treatment was the same regardless of fitness levels – showed that as patients aged, treatment often had to be altered or discontinued prematurely prior to relapse due to side effects, problems with tolerability or through patient choice.
“This is a huge step towards personalised medicine in myeloma.”
The current trial will use the International Myeloma Working Group frailty scoring system to evaluate age, other illnesses and whether a patient can live independently, before categorising patients as fit, unfit or frail. These different groups can then be given different medication strengths.
The trial also explores whether a combination of two maintenance treatments, administered after the initial medication to keep the disease under control, will improve outcomes for patients without increasing side effects.
Sarah McDonald, Myeloma UK Director of Research and Patient Advocacy, said: “This is another great breakthrough in myeloma trials.
“This trial design is great news for myeloma patients, especially during the COVID-19 pandemic, as it gives them the opportunity to have a triplet of tablets at first line.
“This means patients joining this trial will get more home and community-based treatment and it alters the frequency of visits to a hospital for treatment, therefore reducing risk from infection.
“Furthermore, the trial targets older and less fit patients who are often excluded from trials, giving them a chance to access new treatments.
“It also aims to identify the patients who are more likely to stop treatment early due to side effects so they can have their treatment adjusted in advance. This is a huge step towards personalised medicine in myeloma.”
Further information
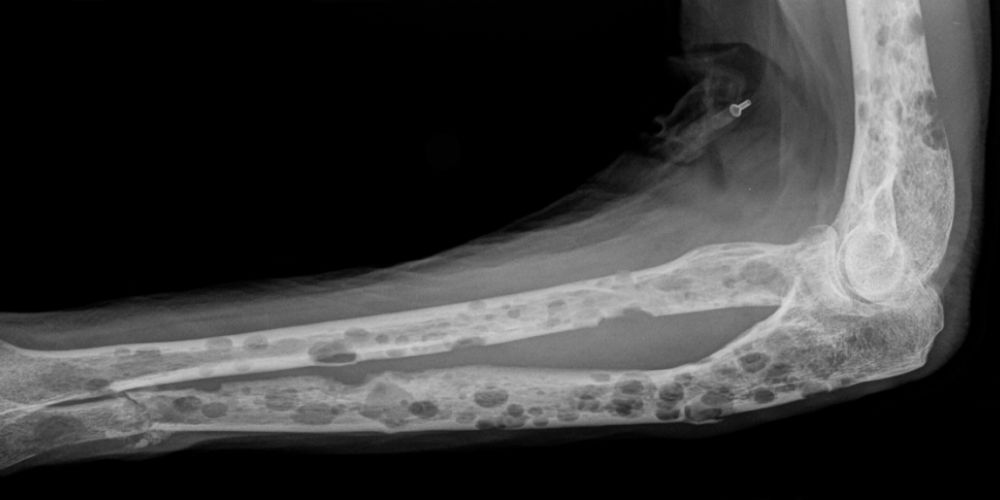
Picture: X-ray with multiple osteolytic lesions in the forearm of a multiple myeloma patient (credit: Hellerhoff / Wikimedia Commons / CC-BY-SA-3.0)
For media enquiries, contact University of Leeds press officer Lauren Ballinger at l.ballinger@leeds.ac.uk