A £7 million research project has been launched to develop a new imaging and keyhole surgery approach to the treatment of secondary bone tumours of the spine.
Known as metastatic bone disease, the tumours spread from a primary cancer located elsewhere in the body. The condition is particularly associated with breast cancer.
The bone tumours cause vertebrae to weaken and eventually fracture, leaving people in severe pain, immobility and requiring surgery. In some cases, the fracture may damage the spinal cord and cause paralysis. For these patients, however, quality of life is a key issue and complex surgery may be inappropriate.
...this project has the potential to revolutionise the treatment of secondary bone tumours.
A research collaboration between the University of Leeds, Imperial College London and UCL has received funding to develop an alternative approach based on developing new imaging and modelling techniques that will enable clinicians to predict which patients are at a high-risk of a vertebra fracturing.
They would then be fitted, using minimally invasive surgery, with a tailor-made implant to strengthen the spine and prevent the fracture.
The project – Oncological Engineering: A new concept in the treatment of bone metastases – has attracted £7 million in research funding, including a £5.6 million grant from the Engineering and Physical Sciences Research Council (EPSRC), part of UK Research and Innovation, the Government-funded body set up to support research and innovation.
Professor Richard Hall, an expert in medical engineering from the School of Mechanical Engineering at Leeds who is leading the research collaboration, said: “The problem facing doctors is they have no way of knowing which of the spinal vertebrae is going to collapse. But when that happens, patients may require major surgery which involves a lengthy period of rehabilitation.
“Our approach is to intervene by developing new techniques and equipment that will prevent spinal fractures, crucially helping to maintain a patient’s quality of life at a time when they may be terminally ill.”
According to Cancer Research UK, 150 people every day are diagnosed with breast cancer. Although more than 76% of people with the disease survive for more than ten years, some patients do develop stage four cancers, of which it is estimated about 50% to 60% get bone tumours.
In stage four cancers, the disease has spread to other organs.
Within five years, the research team hope to have developed new techniques and materials that will revolutionise the treatment of bone metastases.
The approach is based on personalised medicine, assessing an individual’s risk that the spine has weakened so much that a vertebra will fracture. In those cases where surgeons intervene to strengthen the spine, the implant will be tailor-made.
Dr Kedar Pandya, Director for Cross-Council Programmes at the Engineering and Physical Sciences Research Council, said: “Through improvements in imaging and modelling and a personalised approach, this project has the potential to revolutionise the treatment of secondary bone tumours.
“It demonstrates the importance of fundamental research and engineering solutions in developing new treatments that will have a profound impact on people’s lives.”
Predicting the risk of bone fracture
Researchers will develop news approaches to patient imaging and computer modelling, enabling them to track tumour development in the spine over time and how it might be weakening individual vertebra. The information would be compared with the loading on the spine, enabling clinicians to predict which of the vertebrae is at risk of fracturing.
Professor Rebecca Shipley, from the Department of Mechanical Engineering at UCL and one of the co-investigators, said: “This funding will enable us to significantly expand our work combining computational modelling with cutting-edge imaging to better understand how cancers grow and interact with surrounding tissues.
“We are excited to use these multidisciplinary frameworks to understand vertebra fracture risk and ultimately help to improve quality of life for cancer patients.”
Implant from advanced materials
Those vertebrae at a high-risk of collapse would be supported by an implant inserted into the spine using minimally invasive techniques.
The implant would be made from what is called a metamaterial, a material that has uncommon properties that can be fine-tuned to the needs of the patient, for example the material could harden when under stress.
Metamaterials are currently used in the aerospace industry but with advances in 3-D computer printing, the research team believe they could be adapted to provide tailor-made structural integrity to vertebrae at high risk of fracturing.
The advanced manufacturing group from the Dyson School of Design Engineering at Imperial will be developing a novel 3D printer capable of fabricating the intricate implant designs. Their machine will utilise smart optical systems to print photopolymers at extremely fine resolution.
Dr Rob Hewson, co-investigator at Imperial, said: “This project allows us to expand our expertise in the analysis, optimisation and 3D printing of structural metamaterials. By working as part of the multidisciplinary team we aim to apply the new approaches and knowledge to improve the quality of life of late-stage cancer suffers.
“We will also be able to apply some of these new approaches back into the aerospace and mechanical engineering sectors where advanced meta-materials have a wide range of potential applications.”
Minimally invasive surgery
By using minimally invasive techniques to implant the material, the recovery period for patients will be days, rather than weeks or months with the surgery that is required if one of the spinal bones fractures.
The NHS long-term plan for cancer treatment had called on researchers to develop new interventions that would improve the quality of life of patients living with advanced cancers.
It is hoped the new techniques will be applied to other areas of the healthcare sector.
Further Information
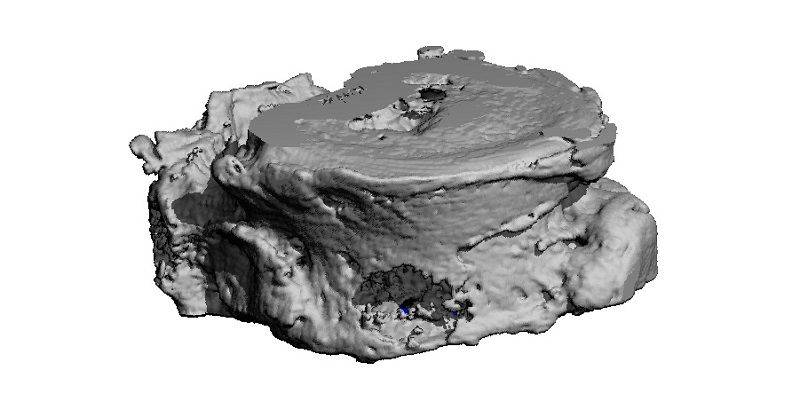
The top image shows a vertebra that has been damaged by a tumour.
For more information, contact David Lewis in the Press Office at the University of Leeds by email on d.lewis@leeds.ac.uk.